
By Todd Krieble and Prince Siddharth*
New Zealand has 20 district health boards (DHBs) for a population of less than 5 million. Because of a lack of transparency, we do not know the costs of administering DHBs. But prima facie evidence suggests it is time to consolidate DHBs and free up administrative resources to use for additional services. In health care, size matters. Returns to scale and quality gains come with size. Optimising governance arrangements and the scale of services means more choice and improved health outcomes as pressures from ageing and public expectations intensify.
The health sector is performing well…
The 2016 Burden of Disease Study, Health Loss in New Zealand 1990-2013 shows that the New Zealand health sector is performing well. Health is improving, but not all age and ethnic groups are doing well. New Zealanders increasingly will have complex health and disability needs. Transitioning to a health system that can respond to multiple-morbidity is a key challenge and will rely on coordination between different health disciplines.
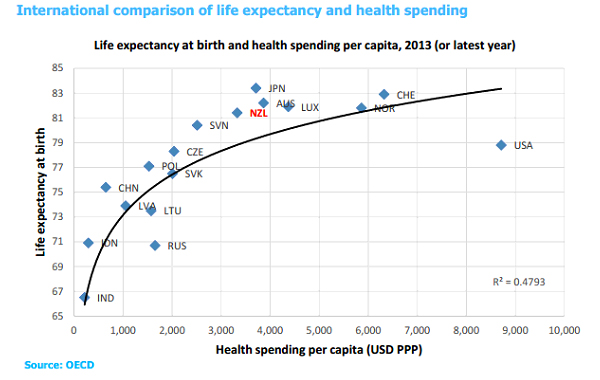
At 9.5% of GDP (including ACC) New Zealand spends above the OECD average on health services – not as much as countries in Europe and North America, but more than Australia. All countries need to optimise expenditure on a constrained budget.
We compare favourably on system performance, with relatively high life expectancy on a modest budget but all systems are under pressure to provide more services and to do so efficiently.
…but there are demand side pressures
A February 2017 report from the New Zealand Treasury on DHB performance states that after several years of spending constraint, several DHBs are under pressure and having difficulty meeting financial targets.
Demand pressures will continue as the portion of the population aged 65 and over reaches nearly 25% by 2050. New technologies and pharmaceuticals continue to expand; and with it expectations of access.
Some groups are missing out
The New Zealand Health Survey shows that more than 25% of the population have experienced unmet need for primary health care. People in low decile neighbourhoods report higher rates of unmet need. The Survey also reports rates of unfilled prescriptions at nearly 15%.
We also know that Māori and Pasifika have lower health status and report significant unmet need.1
Can DHB consolidation free up resources?
New Zealand has many DHBs. The governance and senior management teams have to offer a lot of value to their communities to justify their existence, especially in the smaller DHBs.
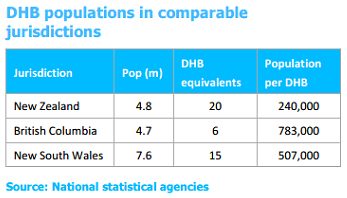
This is because there are obvious trade-offs.
Unless decentralised administration clearly offers better value to a local community, a consolidated administrative approach has the potential to free resources for more local services.
The health care literature shows there are returns to scale and quality from critical mass and regular practice (see for example, Fareed’s (2012) meta-analysis on the impact of hospital size on patient mortality). Several services are managed nationally or regionally (e.g. organ transplantation) to recognise this fact.
Where is the cost transparency?
Getting a clear sense of how much is spent on DHB administration is difficult. Administrative costs are not published in DHB annual reports. The Auditor General in her Reflections from our audits: Governance and accountability report of 2016 provides a set of observations as to the importance of public reporting. She notes that accountability enables trust in government and needs constant attention. This means residents can see how their taxes and rates have been used.
The information reported by DHBs needs to give a complete and accurate account of the use the entity has put public funds to, if DHBs are to meet the spirit of the Auditor General’s observations.
Signs point towards consolidation
The public may be surprised that there are already four regional agencies2 providing shared services with an additional layer of costs and governance. The combined budgets of these four shared services agencies exceed $200m.
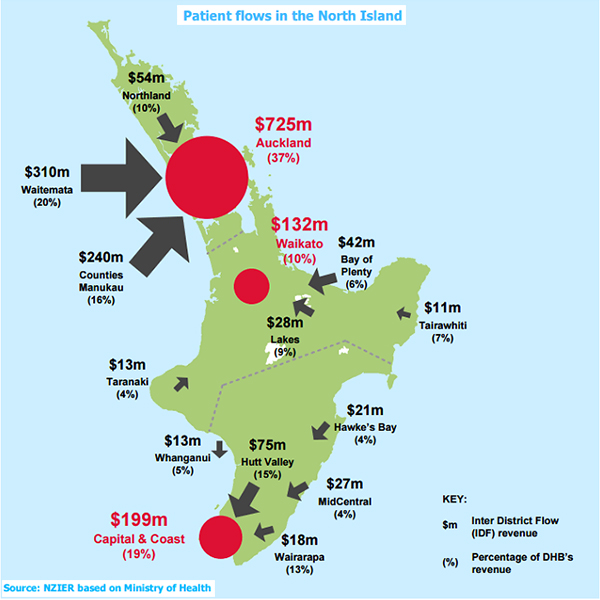
Larger DHBs already provide substantial services to smaller DHBs. We see this in the volume of inter-district flows (patient flows i.e. patients from one DHB receiving care at another). 37% of Auckland DHB’s revenue comes from other DHBs. In Wellington, nearly 20% of Capital and Coast DHB’s revenue is from other DHBs.
These patient flows add a further administrative burden to the system because these transfers must be counted, costed and reimbursed each year. Small DHBs have to negotiate access.
Health Ministers have also appointed board members to more than one board. This serves to enhance coordination between DHBs and is a further signal that DHB transaction costs could be reduced through consolidation.
How valid is the claim that DHBs are about democracy and local autonomy?
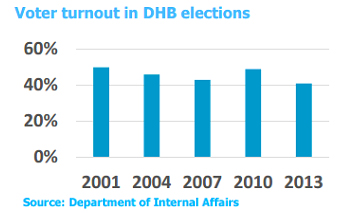
Voter turnout in DHB elections was 41% at the 2013 election.
Turnout ranged from 34% to 55% in 2013 with smaller DHBs recording higher turnout.
DHBs are only partially elected with room for four ministerial appointees alongside the seven elected members. This makes for 220 ‘governors’ across the DHBs.
The 2015 New Zealand Health System Independent Capability and Capacity Review noted that DHB governance and leadership competence appears to be “lacking in practical day-to-day execution”. The Review recommended a reduction in the size of the boards.
Health services are complex but DHBs have very sizeable funding, reporting and service change approval requirements to the Minister and Health Ministry. Funding is from the centre and not locally raised so financial accountability is straight back to Wellington as the source of funds. Local district health board discretion to alter or change the service mix is limited. Any significant changes require consultation and approval with Ministers. On matters of national infrastructure (i.e. ICT), negotiations are often required with each of the 20 DHBs. As new digital treatment technologies emerge (e.g. in-home screening) the need for local discretion is non-existent or very limited because a nation-wide system has to be able to talk to itself to offer consistent and coordinated service.
What next?
DHB and shared service agency administrative costs need to be collected and reported in order to meet the spirit of the Auditor-General’s reflections on good public reporting. Transparent costs are needed so the local governance costs, local administration costs, patient flow management costs, and regional coordination costs can be contrasted with the potential to free resources for additional services and to reap the returns to scale and quality. This is especially important when we have under-served populations that report access barriers to primary care. If consolidation of DHBs frees up resources for more services, then we think it’s worth a closer look.
This Insight was written by Todd Krieble, Principal Economist and Prince Siddharth, Economist at NZIER, May 2017.
6 Comments
What about 1 DHB?
Totally agree.
NZ Inc needs 1 National HB (monopoly) and many providers (competition) to minimize the costs and maximise the service & service levels. (Effectively Pharmac but for treatment).
NZ Inc doesnt need to own the hospitals just the service requests. NZ Inc would need to manage the Herfindahl index (https://en.wikipedia.org/wiki/Herfindahl_index) to provide strong competitive levels (maximised service) - no oligopoly providers
Hospitals can bid for any one that gets sick - for this to work the required service levels have to be high to avoid cheap and nasty.
Even GPs can be on the same basis. If a person waits to see a specific GP then they pay any premium over the bid rates.
For emergency services, yes the nearest hospital will have to treat but it will be on the basis of bid prices. The National Health Board would have to act something like transpower & set rules for determining how these would be priced.
Technology is now good enough to have a centralized bid system. Yes it would require massive categorisation of treatments, but could start small in one area of health and grow to cover the system.
I work all day every day with DHBs. They are absolutely operate in chaos. There is no management, rather it's just political warfare, or unlimited workarounds to avoid that.
I see no indication that increasing size will change that. It's not size, it's inbred culture.
Let's compere this proposal with the amalgamation of 7 councils into one Auckland monolith. Care to speculate just how badly those outside the "city" fare? Answered - "This is especially important when we have under-served populations that report access barriers to primary care"
"....the scale of services means more choice and improved health outcomes as pressures from ageing and public expectations intensify." Does this include the mass immigration, the tourists that are not required to get travel insurance in this country - or just the easily said - aging population mantra?
"The National Health Board would have to act something like transpower & set rules for determining how these would be priced." How is this working for the consumers of electricity - or patients in this case?
A competition for health funding - cough - outcomes between the huge city of Auckland and the provinces - no thank you!
Another consultant borrowing the DHBs watch to tell them the time. The sector is tired of people who have not worked in it giving their opinions. From my 16 years working inside the system effectiveness and efficiencies are constantly being promoted and the best results are achieved when they are implemented by management following Board scrutiny and sign-off. So lets just let them get on with this. The sector has also had enough organisational reviews and paid out millions of dollars to consultants for the priviledge with mixed results, often when the recommendations only replicate what is being worked on/implemented internally. Thanks but no thanks to this opinion
Further to the above, if NZIER wish to make a difference to the public health sector in a positive way it could look closely at the cost to publicly funded health services of treating overseas visitors who for a number of reasons do not pay for their care. With tourism numbers soaring and the ability to further reduce costs in the sector limited, the 200m pa NZIER claim could be saved in the back office would be much more easily achieved in this area. They should work with the MOH, and Ministers of Health and Tourism to identify the reasons why costs are not currently being recovered and lobby on behalf of the sector to recover this revenue. Their opinion on this subject would be well received
We welcome your comments below. If you are not already registered, please register to comment
Remember we welcome robust, respectful and insightful debate. We don't welcome abusive or defamatory comments and will de-register those repeatedly making such comments. Our current comment policy is here.