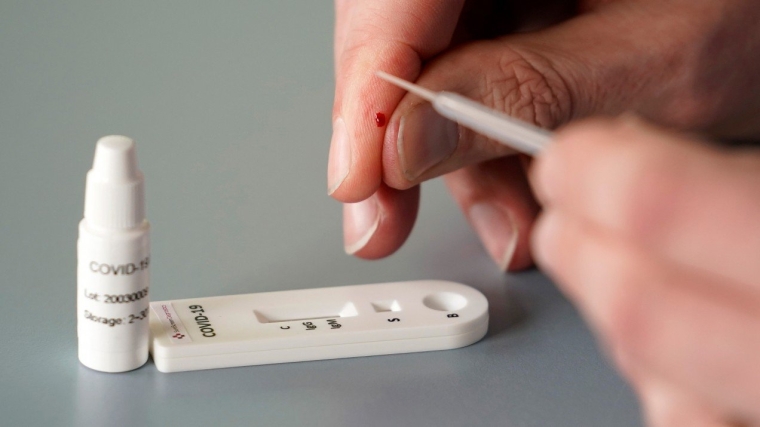
The fundamental problem facing COVID decision-makers is that they are flying blind owing to lack of testing data. This will become even more crucial as we head towards the end of the four-week lockdown and have to decide when and how restrictions can be gently lifted.
The first necessity is to work out exactly where we are. We won’t get to that knowledge-point without some improvements to the monitoring equipment. The best but currently unused weapons are newly-designed quick-fire serology tests.
First, it is important to acknowledge that the latest (April 3) data gives scope for optimism. It is not only that the total number of new cases was only 71, with this being a decline from the previous day’s 89. More important is that the number of positives has not tracked up with the number of tests being conducted.
A week ago, there were days where we were getting one positive test for each set of 20 tests conducted. The last number of 71 positives from more than 3400 tests is approximately one positive per 50 tests. That is definitely good news.
Another piece of good news is that the slope of the epidemic curve has not increased since we went into lockdown on 25 March. Essentially it has straight-lined rather than exponentiating. If and when it starts to curve over and flatten then it will change into what mathematicians call a Gompertz curve.
Apart from madmen and a few economists, no-one believes that exponential growth can continue indefinitely. It will eventually turn into a Gompertz curve. The challenge with COVID-19 is that left unchecked, the exponentiation can continue for a long time and this is what we are now seeing in many parts of the world.
The fact that in New Zealand the curve stopped exponentiating so quickly is encouraging. It tells us that the pre-lockdown measures have already been having some effect. However, there is still a chance, albeit decreasing, of new super-seeding events emerging and another exponential wave occurring. Also, we don’t really know at all what is hidden within the community.
We are now getting close to the date when we should see a clear declining trend in the number of new cases per day. The next three days will tell us if we are looking at a real downward trend or just being teased by volatility in the data.
The risk has always been that the number of positives was being artificially lowered by lack of testing. That risk is starting to lessen, but we are not in the clear yet.
A key message in all of this is that we are still stumbling around in the dark not knowing where we are.
Director of Health Ashley Bloomfield has said that he wants to see some movement toward surveillance testing. That means testing cases that don’t necessarily fit all of the criteria. However, although Bloomfield has not stated it, the PCR test using swabs is an expensive and indeed clumsy way of doing this. The answer lies in serology.
Whereas PCR testing of swab material searches for the virus, serology (blood) tests look either for antibodies or specific proteins in the blood. At this stage it is the antibody tests that are ready to go and indeed are being used overseas. A big advantage is that some of these new tests are cheap and can be rolled out at scale. For example, I have seen a quote from a New Zealand firm, already working with Government on another project, that can supply these at under $7 per test, with 100,000 tests delivered within a week. One further week, and everything could be operational.
Because these antibody tests are new, some caution is appropriate at the level of individual cases. However, the validation tests that I have seen show excellent sensitivity and specificity. In other words, the levels of false positives and false negatives are very low.
Of course, nothing is absolutely sure with new tests until they have been rolled out at scale, and so a little caution is appropriate. However, PCR tests also produce false negatives, indeed a great deal of them, and that is why we have a ‘probable category’ for cases where the test did not find the virus despite clinical evidence that it is present.
A big advantage of these new serology tests is that they are quick and, unlike the current PCR tests, can be undertaken without laboratory procedures. Any clinician can get a quick answer within 15 minutes using a spot of blood from a pin prick.
Accordingly, these serology tests are excellent as a filter of cases which are probably ordinary flu but for which there is uncertainty. They can also be used with close contacts to identify those that need to be quarantined more stringently. Even more important, they can be rolled out as a surveillance program at the community level.
Right now, we have some apparent hotspots in New Zealand. Taking Queenstown as an example, the whole population could be tested over a few days from a mobile testing station and anyone coming up positive put under quarantine. One of the good things about these tests is that they have potential to pick up cases prior to symptoms and before it is possible to obtain positives from the swab testing.
If no-one comes up positive apart from those who have recovered from the disease (and will therefore have the antibodies) then we know there is minimal hidden community transmission.
Another potential use of serology is to test development of immunity at the population level. Alas, despite some media suggestions to the contrary, the international evidence is that we should not expect to see much evidence of antibodies and hence COVID-19 protection beyond those who have been infected with symptoms at some level. But we need to find out for sure.
To date, I have seen no mention from the Director of Health, nor any questions from the mainstream journalists, as to what New Zealand is doing in regard to serology testing. I suspect the reality is that we are doing very little.
That situation may be linked to the reality that most Ministry of Health staff will be pre-occupied with operational issues. Ministry of Health is unlikely to have many staff with serology expertise. These types of people tend to not be found in the bureaucracy.
Accordingly, it is time for our Prime Minster to ask the Ministry of Heath to set up a group to report back within 72 hours as to the pathway forward. Alternatively, the Prime Minister’s Chief Scientific Officer could be tasked to manage this.
Perhaps the best way forward would be to direct the request directly to Professor Sir David Skegg to organise, given that he has both the professional expertise and a long history of working alongside Government and bureaucracies. Professor Skegg has been appearing before Parliament’s Epidemic Response Committee this week where he has called for greatly increased testing and contact-tracing.
Whoever is appointed, and whoever that person co-opts, this is something to be done urgently.
There are actually two parts to the what is needed. One part is to quickly evaluate the firms that claim to have suitable certified tests and who can supply now at scale and a reasonable price. The second part is to design how serology and PCR testing of swabs can complement each other within an integrated program.
In New Zealand, we are in an internationally unusual situation in that we still have a realistic chance of stamping out this virus before it totally takes over. In that regard we are in a different position to almost all other countries. Accordingly, in finding the path from Level 4 to lower restriction levels we will have to do our own thinking and planning.
In recent weeks, comparisons have been made between ourselves and the East Asian countries of South Korea, Japan, Hong Kong and Singapore. There is no doubt that those countries all managed to flatten the curve. Unfortunately, it is also now clear that they have not stamped out the virus and that they now have to stamp harder as a new wave of exponentiation is building.
As for countries like Sweden, the Netherlands and Belgium, all of which have tried to minimise disruption to normal life, they are all in big trouble. Their trajectories are all consistent with Italy and Spain, and only about a week to ten days behind on a per capita basis. The implications of those relaxed policies, now with rapidly increasing death rates, have become increasingly evident.
In recent days, our leaders have tried to deflect criticism of insufficient testing by saying that the international calls to ‘test, test, test’ do not actually apply to us as we are already doing lots of testing. Well, we are doing lots of testing but we need to do a lot more if we are to come out of lockdown as early as possible. That’s where serology fits in. Let’s do it!
*Keith Woodford was Professor of Farm Management and Agribusiness at Lincoln University for 15 years through to 2015. He is now Principal Consultant at AgriFood Systems Ltd. . He can be contacted at kbwoodford@gmail.com. Keith’s previous COVID-19 articles are available here.
175 Comments
""A week ago, there were days where we were getting one positive test for each set of 20 tests conducted. The last number of 71 positives from more than 3400 tests is approximately one positive per 50 tests. That is definitely good news.""
Not Really
a week ago (and before that) we were only testing the most severe symptomatic cases, and to a large extent only those cases which could show a connection to an international traveller, plus there were not many test kits available.
Now we are testing anyone that turns up, and in much larger numbers due to greater test kit availability.
These factors have distorted your reported results and your assumptions
RCD,
If you look again those are exactly the issues I am addressing.
KeithW
There is some truth to what you are saying ( the testing criteria have changed leading to change / reduction of bias in the sample .. ) but you are exaggerating far too much .
We are definitely not "testing anyone that turns up" ( which would be a good thing of course ) so Keith's reading of the results is likely correct.
If the criteria and the selection is variable and insufficient then the figures produced obviously are questionable. Still some useful patterns have nevertheless emerged. One of which is undeniable in that actual hospital admissions still number less than twenty. Therefore that must be encouraging because it means that the resilience of afflicted NZrs and the robustness of their immune systems is coping. They are self healing in other words and the vulnerable elderly and pre-existing conditioned are doing well too in keeping out of harms way. On that basis alone, could we not say so far so good.
My understanding is that somewhere between 5 - 20% of infections are bad enough that people need medical treatment and hospitalisation. If we had a lot of undetected community transmission, we'd be getting a lot more hospitalisations.
Tks Doris, exactly, it is a telling point that we should all be noticing because it speaks for itself, and it should be, so far at least, of some comfort.
Do we conclude that 80 - 95% of infected people go unaccounted for?
This is possible ( although I am with Keith in thinking it is probably more like 50-70% in NZ ) .
Let us say it IS 80-95% as you say - a rather stark contrast with your persistent suggestions here and elsewhere that it is actually 99% ( corresponding to factor 100 infection under counting ). Do you still think it is 99% or near that ??
RCD as far as I remember, the MOH has been saying very clearly from Feb that they have no capacity issues. They have said this repeatedly, so why you say that they were short of testing kits? I never, ever seen (please correct me if I am wrong) a single statement by any officials, in MOH or otherwise, that they do not have enough kits or any other capacity issues.
Believer 1980
You are correct in regard to the statements from MoH.
But those statements do not align with the real situation that has existed in recent weeks.
This is because the first response of the MoH when they are asked difficult questions is to fudge.
Ths is standard bureaucratic behaviour, and when situations become impossible to refute in the light of evidence, bureaucracies then acknowlege situations in relation to the past but say that everything is now all OK.
This is how bureaucracies maintain 'social licence' for what they are doing (in the short term) but it is also why citizens become cynical about their governments (in the longer term).
Keith
You mean 'social licence' equals 'poetic license' as in the first casualty in a war is the truth?
Believer 1980
You are correct in regard to the statements from MoH.
But those statements do not align with the real situation that has existed in recent weeks.
This is because the first response of the MoH when they are asked difficult questions is to fudge.
Ths is standard bureaucratic behaviour, and when situations become impossible to refute in the light of evidence, bureaucracies then acknowlege situations in relation to the past but say that everything is now all OK.
This is how bureaucracies maintain 'social licence' for what they are doing (in the short term) but it is also why citizens become cynical about their governments (in the longer term).
Keith
“citizens become cynical” how sadly true that is. NZ has quite some issues with its bureaucracy as is being explained in this column today and also for instance the overbearing and punitive persona adopted by EQC during the Canterbury EQ crisis. Bureaucrats used to be known as Public Servants but that that accurate & inconvenient moniker was long ago discarded. A bureaucracy that is unaccountable, opinionated and self serving cannot help but undermine both democracy and society.
There is multiple reports of doctors from clinics ordering 30 test kits and receiving 2. If no capacity issues, why was this happening?
I also think that it was a shortage. Just that MOH was misleading us and blaming others. See Keith response above. As an immigrant coming from a country with no democratically elected government, I was just expecting more from a democratically elected government, in a small country with well behaving citizens who listen to authority (by and large) out of their own belief (and not fear). Why they do the exact same thing as the authorities of my old country? This is more frustrating than anything else. I struggle to understand the motivation behind such a blatant denial of truth and shifting the blame to others. I am also disappointed that NZ population does not hold the politicians in check and accountable. Even in a situation like this! everyones life (biological and economic) is now affected by our government decisions. Yet people (by large) show no scrutiny of decisions made. no demand for transparent information. Maybe this is becasue the alternative (National) as just as bad, so what is the point of you wasting your time when at end of the day, if you conclude that JA is unreliable, dishonest politician, you will have Simon Bridges as the alternative and you know that he is probably even worse!
It's called human nature
Oh, but it was the clinicians decision to not test anyone who has not been overseas in the past 14 days, or been in touch with a known COVID19 patient. So we really have to blame our community doctors who have failed us according to our top elected official the prime minister.
NZ government has failed to communicate clearly and honestly what they are doing to battle the virus from the get go. JA is one of the least transparent leaders I have ever seen, right up there with John Key. It is only natural that we see the MOH response to the issue so confused and unclear.
We have been going blindly but it seems (and I really hope) that we have been exceptionally lucky that we did not end up like other English speaking countries. As we did exactly as they did (i personally think NZ has been simply looking up to the UK, what they say, what they do and copy them, So our true leader is Boris Johnson! terrible news to me)
Believer1980
I would be cautious about blaming the clinicians. Often it has been the testing centres that decline to test despite a clinician's request. Also, the testing centres are hamstrung by their own logistics. Our Prime Minister is wrong when she keeps saying that the low testing was because of lack of clinician referrals but this is because MoH have been feeding her incorrect information, linked to their unwillingness to acknowledge their own logistical issues, and poor internal messaging from MoH to the testing centres.
KeithW
.
:) i totally agree. I was being sarcastic Keith. It was very poor form from JA to blame the clinicians when they got clear instructions from MOH as who to test. MOH has not clearly communicated their testing plan and regime from the get go. They might have an excellent plan given the parameters they know, but they did not share it with us, they did not share those parameters. So, in absence of competent, honest and transparent communications, we all remain confused and rightly highly critical of MOH.
No knowledge of how soon after infection antibodies are detectable??early testing may give false negatives?when do you test
kiwichas,
One of the strengths of serology is that you can afford to test each day if you wish, and then get a result on the spot. It is ot yet totally clear as to how much earlier quick-fire tests will find the virus compared to swabs and PCR, but it does seem evident that they can typically get it a day or two earlier.
KeithW
There is some commentary out of the US now about why California shows a statistically much lower number of cases and deaths than New York.
The idea is that the Coronavirus was circulating much earlier than has been indicated by China, as long ago as July/August last year, and due to the large Chinese population and high level of Chinese tourists this virus has been circulating there for a long time and presented a higher number of "flu-like-illnesses" and some deaths with the result that some Herd Immunity has already occurred there. They argue that this may not have occurred to the same extent in New York, i'm not saying it is true, just passing on the comments and theories.
But, looking back at NZ 2019 Flu history we also seem to have had a particularly bad flu season, ran out of flu shots, and had many more cases even though many more people were vaccinated, so, maybe, in our case given that we also have a significant Chinese population and a very large historically number of Chinese Tourists, maybe, NZ has already had a dose of this and it passed under the radar and we have some immunity already.???
The test kit for Antibodies (to see if you have already had it in the past) may deliver eventually some interesting numbers on this issue.
Good call. Is it the same scenario in Australia as they have a very similar infection rate and low death rate
Extremely unlikely, given how fast this virus spreads. From 1 person to entire planet infected in 60 days if unchecked, in mathematical models.
Misses the point. Exactly and completely
You should really read more. This theory debunked, see Keith's comment below, already tested old samples and no trace.
Houseworks is part of the tin foil hat brigade.
FACT: NZ and oz have statistically lower death rates too. Actual infection rates are broken down too and they are way lower than the promoted rates. See below. There is no need for insults, as members of the public we are all trying to understand this. NZ Officials and ministers should have their fingers on the pulse but they dont and have dropped alot of people in unnecessary crap
"There is no need for insults."
That's rich coming from you. Just in case you can't find it Houseworks, go up 3 posts for your ad hominem .
On the herd immunity theory, LA vs NYC I pointed out elsewhere you could just as easily conclude the difference lies in the difference in density between the two cities. But, neither does that make the density theory true. If anywhere is going to give us an indication about herd immunity, I suspect it would be Wuhan we need to look to now their boarders are re-opening;
https://www.theguardian.com/world/2020/apr/03/coronavirus-wuhan-residen…
Oddly, the government has just told them to "stay inside, we're about to re-open the boarder". So much for herd immunity theory.
At present NZ has a much much lower than 1% mortality rate.
Yet we are destroying the economy and society.
Society seems ok here...even improved
RCD,
The Chinese have gone back and tested some thousands of stored blood samples collected for other reasons in November and December and found no evidence of the virus circulating then in the Wuhan population. The Californians could do the same. My expectation is that they would get the same result as the Chinese. The evidence suggsts to the disease beoing present in Wuhan fish market workers by about 10 December or a little earlier, but there is no real evidence that this was where it originated. Rather, it was probably one of the very first super-spreading events, but almost certainly there were other unidentified clusters starting to emerge in Wuhan by then or very soon thereafter, given the speed of the subsequent contagion.
KeithW
Keith what do you make of the research indicating that the US has the most diversity of strains of the virus thereby implying it originated in the US and was exported elsewhere.
Rosenstein
I have no factual basis on which to comment either way. I would need to see the evidence in relation to strain multiplicity. But I have some inherent scepticism, given other circumstantial evidence, that it originated anywhere other than in Wuhan.
KeithW
It's an unpopular avenue of research, you may get lit up for referencing this research paper, but science is better than hearsay.
"Decoding evolution and transmissions of novel pneumonia coronavirus (SARS-CoV-2) using the whole genomic data"
https://www.researchgate.net/publication/339351990_Decoding_evolution_a…
Rosenstein,
Yes, this is certainly an interesting paper. It seems to confirm that the Huanan fish market was a super spreader rather than the original source. I will need to go through the paper again looking at the evidence relating to the phylogeny and the ancestral types, and where that evidence leads.
KeithW
Well thank you for taking the time to read it and reply - you must be a busy man. Much appreciated!
You really believe what the Chinese say to cover theirs collective Arses.?
If California did the same test that i would believe
Keith
You are probably right, there are major density and Mode-of-transport differences between NYC and California which can account for the spread difference, not so sure about the death rate difference.
Possibility still exists that a different strain of the virus came through back then and now it has mutated to a much more powerful version.?
Not sure if antibodies from an earlier version would still be effective against the current one.
"Twenty five billion dollars to test the entire US population. Now suppose the pandemic knocks 5% off US GDP over the next year or two, that’s roughly a trillion dollars lost. Or to put it differently, $3 billion a day. Thus, if mass testing reduces the number of days we are away from work by 9, it pays for itself. Let’s again be conservative and say that testing will also require a $25 billion fixed cost to build the enzyme factories and so forth, for a total cost of $50 billion. 18 days and it’s worth it."
https://marginalrevolution.com/marginalrevolution/2020/03/a-solution-if…
"We propose an additional intervention that would contribute to the control of the COVID-19 pandemic and facilitate reopening of society, based on: (1) testing every individual (2) repeatedly, and (3) self-quarantine of infected individuals. By identification and isolation of the majority of infectious individuals, including the estimated 86% who are asymptomatic or undocumented, the reproduction number R0 of SARS-CoV-2 would be reduced well below 1.0, and the epidemic would collapse….Unlike sampling-based tests, population-scale testing does not need to be very accurate: false negative rates up to 15% could be tolerated if 80% comply with testing, and false positives can be almost arbitrarily high when a high fraction of the population is already effectively quarantined."
Profile
By my reckoning is would coat about $US1.5 billion to test evryone in the US and about $NZ35 million for all of NZ. This is the cost of the tests and does not include clinicans (doctors) time. But right now doctors in NZ are not exactly busy as all of the normal contagious diseases have also been stopped in their tracks.
KeithW
Thanks Keith. That sure is a pittance compared to the current cost in lives, jobs and the economy, due to the lockdown.
"The first necessity is to work out exactly where we are. We won’t get to that knowledge-point without some improvements to the monitoring equipment. The best but currently unused weapons are newly-designed quick-fire serology tests."
Currently unused weapons Wtf. We have a group of fluffy talk do-nothings that dont deserve to be in government leading the country. JA pulls out a stream of platitudes and witty slogans with absolutely nothing behind it. Wake up and get effective because right now I feel we're paying an extremely heavy price for your lack of effective action at the border.
We will certainly need to scale testing substantially to get the quality and resolution in data that will be required to make meaningful descisions. For example, going forwards, we cannot lock down the entire country because there is one community transmission event in Queenstown or Auckland. If that means we need industrial scale automated testing that equipment is already available globally.
What we do not have is the luxury of time. Once a month has passed I expect that social distancing measures will have fatigued and people will stop abiding by the rules. Talk of extending quarantines and "No plan B" is entertaining a fantasy that is neither realistic nor economically viable. Testing needs to be fit for purpose when we have to take the brakes off.
Keith, yet another great article, I'm rapidly becoming a big fan of yours.
Indeed we really don't know how many people are infected in NZ because we have tested so few (I believe less than 1% of the population, correct me if I'm wrong). Therefore it is likely that the number of infected people in NZ could very well be 100 time higher, i.e. 80'000 because most display no symptoms of having CV. If this is the case, do we still believe we can eradicate CV by isolation? It's extremely doubtful given the the virus' infection rate. If that's the case we have no real plan to beat CV but to delay it.
We indeed need lots, lots more testing!
Some may be alarmed by my comment that we could currently have 100 times more infected people in NZ that the 800 reported. This is not necessarily terrible news because if that's the case (and it would apply to other countries as well), it means that the death rate as a proportion of infected people also reduced by a factor of 100. We currently have 1 death for 800 infections = 0.1% death rate (this rate could of course rise), if there are indeed 80'000 people infected the current death rate becomes 0.001% If this is the case we should really reconsider if it's not best to let the virus run it's natural course (it may anyway, despite the lockdown) as it is recognised that generally 40% of the population will naturally never get the virus and 0,001% of 5 million people x 60% in NZ is 30 deaths
As far as I know NZ is the only place that has only been testing income passengers. Not sick people (pretty much everywhere else). As a consequence, we have got a case portfolio of younger infected people, with the majority having a mild case. Sad enough, the only death was an old woman who was not tested (as she was not a recent traveler or in contact with a confirmed COVID19 case).
So NZ does not have a full picture (the spread that affects a community with the age and health condition of the average person living there). So results cannot be extrapolated to NZ wide population in any form. This is why we needed a testing plan that would have informed us what is going on in our communities. Yet, not only we are not testing people in the community as up to now, we have been refusing sick (and very sick) people with flu symptoms until very recently (and I am not sure if that has changed yet).
NZ must have one of the worst testing regimes in the whole world. The only other country with such a poor testing regime that I know off is Iran.
"NZ is the only place that has only been testing income passengers"
That's not correct B1980
It is not 100 times higher.. not in NZ , not anywhere else . There is not a iota of evidence for it.
Best estimates , supported by data come out at 2-10 times under reporting of infections rates depending on the number of test / testing criteria.
You are dreaming ...
Pashaas, I wasn't suggesting infections are 100% higher, I suggested 100 times higher = 10'000% higher. There is indeed not a iota of evidence for it, nor is there a iota of evidence that there are only about 800 infection in NZ, because less than 1% of the population has been tested, and that was my whole point. How do you know you haven't had CV? You don't
Typo on my part - I meant "100 times higher" ; corrected now.
Where you are wrong is ".. nor is there a iota of evidence that there are only about 800 infection in NZ, because less than 1% of the population has been tested" . The data we have is not complete , and the results/numbers we have from it are not definitive - however they are not meaningless , unlike your suggestions / dreams of 100 times higher rates / pre-existing immunity - those are just dreams.
paashaas, how do you know you haven't had CV yet?
I do not know that. What is your point ?
My point, as per previous post, is that we have no idea how many people have CV in NZ
That is plainly false. We do not know exactly - it does not mean that we have no idea. We do have a plausible range of estimates .
I am sure that you of all people have a pretty good idea of what your house is worth :) - despite not knowing it exactly.
Your suggestion that we currently have 95k infected people in NZ ( 100 times the current confirmed cases ) is way outside the plausible range.
How do you know only 1 person in NZ has died from it as well?
Death Certificates, they can be easily counted, are accurate and include "cause of death"
Yvil,
So far we have tested around 0.6% of the population (roughly 30,000 out of 5 million).
I don't think the number of infected people is anything like 80,000 but it could well be 1500 or 2000 rather than the current confirmed plus probable numbers of 800. Either way we need to find out.
KeithW
"The fact that in New Zealand the curve stopped exponentiating so quickly is encouraging. It tells us that the pre-lockdown measures have already been having some effect. However, there is still a chance, albeit decreasing, of new super-seeding events emerging and another exponential wave occurring".
So what happens after lockdown? Especially when this new virus already looks to be mutating to a more virulent strain effecting more of the populations age groups: CNBC: WHO says ‘more and more’ young people are dying from the coronavirus. "It is a mistake to believe that the virus only severely impacts older people and those with underlying conditions, said Dr. Mike Ryan, executive director of WHO’s emergencies program".
https://www.cnbc.com/2020/04/03/who-says-more-and-more-young-people-are…
CJ1099
Your question as to what happens after lockdown is exactly the reason why we need a lot more testing
KeithW
We were not doing enough tests, despite all this "capacity" waffle.
Should be testing at random (like a poll) and then see what % of pop has it when extrapolated .
Then, start quarantining those positive. NOT isolating, QUARANTINE
Case totals probably 6 times under true total.
Does not help that DoH keeps repeating that asymptomatic are not really a danger and don't need testing , despite fact that they are acknowledging to be spreading it pre infection.
When we move back to level 3 everyone with so much as a cold or cough will need to be tested because transmission will occur at a higher rate and we are heading into flu season. For randomised community testing and surveillance the fastest and cheapest way is likely an ELISA.
We should start contracting and training the hundreds of people required to collect samples and conduct that testing immediately. All the technology and physical resources are available but getting the people will be slower.
Yes, Keith the deficiency were everywhere, no one knew how this Covid-19 on last Nov.- so all can be forgiven, to wear a mask or not?, to use full PPE gear or not? (just a normal A&E PPE cover, face shield?), you can see stock preparation of full covered PPE gears at South Korean hospitals, to ensure that not a single tiny droplets expected to be in touch with the Doctors/Nurses, now compare that to those in Italy & Spain, they're in much better healthcare systems comparatively with NZ, so this going hard lock-down by Jacin - is the only way. I worked in couple DHBs for years - so knew very well, we're just/won't cope if this bugs hit our nationwide hospital in Tsunami fashions - Our healthcare troops is the secondary, next to the ICU patient at their care. This will be natural event worst hitting us than the flaw decision on landing the troops ashore to be slaughtered - except, we are right now.. in better advanced warning system...to avoid it ..please..at any cost.- Ask any Pathologist & check those worldwide presentations how quickly this Covid-19 overcome the lower respiratory system. Honestly, they're like a rock stars.. in very short time convincing the audiences to be like one of them.
Keen observer,
I believe you are saying that you agree with the lockdown because the alternatives are very bad. That is my own position also. However, I think we know that this virus can play many tricks to keep ahead of us, and that is why I believe we do need to be identifying all of the deficiencies as they currently exist. It is normal for bureaucracies to act slowly and at times like these that can be disastrous. The reality is that we did not have good systems in place. That is exactly how it also has happened with the Mycoplasma bovis campaign over the last three years, where it took at least two yars for MPI to get reasonably up to speed, and during this time they fed us with a lot of BS as to what they were doing and achieving, all self-justified by the importance of maintaining 'social licence'.
KeithW
If any advice from the leader of NZ's People's United Party was taken seriously, NZ would have been in a much much better position.
Advice from this government is about two weeks lagged. they are typical followers not leaders.
Never heard of it. Is that some coffee group you have appointed yourself Chairman of?
The Pup party?
Yep, pisses on the carpet and still expects to get treats.
We're have you been hiding X? We have been missing your CCP authorised posts lately. Hope you are coping with the lockdown.
The government needs to announce now. That when this is all over. Whichever way it goes. There will be a Royal Commission of Enquiry into the Ministry of Health response to the Covid19 pandemic. Everyone involved needs to know right now that everything they have said and done so far and everything they say and do from now will be subject to full scrutiny at some stage in the future. Then they will start behaving and acting in all of our interests.
Totally agree about a royal commission. But not to find scapegoats. With very fuzzy evidence important decisions have to be made. Quite likely many mistakes are being made ut what matters isn't who is making them but what has to be in place to avoid them in future.
Incidentally my guess for low numbers of testing is a decision was made to retain testing capacity just in case things got much worse much faster. Now with hindsight we can complain but it may well have been the right decision at the time it was taken. Now why did we (and some other countries) have restricted testing capacity - was it over-trusting WHO and if so what do we do about it?
Turkeys don't vote for Thanksgiving.
Keith
If I read you right and if the pinprick test can be self-administered (daily), then surely, if the result of those pinprick tests identify "any" abnormality then that person can hop off to the testing station pronto. $7 a pop is pocket-fluff
The test doesn't need to be absolutely conclusive, just indicative of an abnormality
Iconoclast,
I beleive these tests are best done by a doctor or nurse under appropriate sterile conditions. Nurses could definitely do them, and put the results into the national system, with perhaps a doctor signing off the result. There are two types of antibody that can be tested for, and each can give a quantitative result with the appropriate reader.
KeithW
Someone told me that the CV test being used is not specifically for the Covid19 virus. It's a general test that can pick up other similar strains as well as covid19. Hopefully I have explained that correctly. I dont know if that's true but it seemed very plausible and only casts more doubt on results.
Houseworks,
I don't think that is correct.
The current PCR test is very specific to the genetic sequence of COVID-19.
Within COVID-19 there will almost certainly be minor variants of individual base substitutions within the code. The standard test will pick all of these, but identifying the specific variants wihtin COVID-19 requires detailed sequencing that is not routine- it is a big job well beyond the capability of the standard laboratory.
In summary, the COVID-19 test will not get confused between this virus and other flu viruses that circulate in the population, but it will pick up COVID viruses with minor base substitutions that all fit within the COVID-19 grouping. Whether some of these variants are more virulent than others is a question that I don't think we currently have any answers for, but it is an important question.
KeithW
Apparently the test kits are tracking coronavirus not covid 19 according to my mate they're two different things. It's quite confusing with all the contradictions
Houseworks,
I am confident your mate is wrong.
Yes, there are many coronaviruses, including some which can cause the common cold, although most common colds are rhinoviruses, not coronaviruses.
The COVID-19 test does not get confused by these other coronaviruses or indeed any other flu viruses.
KeithW
Thanks keith for the great info.
The PCR testing is specific to the virus RNA so it's very unlikely you'd have a false positive. ELISA testing is specific to viral proteins so it is possible you could get a few false positives that might require further investigation.
Keith - question: global deaths so far around 50k versus 500k for flu every single year. Would you suggest we shut down the global economy for a couple of months every year to combat the flu? Seems like a sensible question to me, but all the so-called “experts” cannot/don’t want to answer it.
The question would make sense if 50K was the end of it .. or even if we expected 500K deaths from letting Covid19 run unchecked.
That is not the case - the best estimates of worldwide death tall in that scenario come to 30-60M within a year .
Those estimates are going to be proven to be utter nonsense, but there will be no accountability from politicians or health professionals when the Imperial model and others are exposed as a bad joke. The hundreds of thousands of suicides that will result from this globally will not be reported. What a joke.
"Those estimates are going to be proven to be utter nonsense" - any evidence to support this statement ?
That his been comprehensively debunked.
The main problem with the article is the same wild/false assumption Yvil is making above , namely that the infection rates are currently 100 times higher than cases confirmed by testing . It is nowhere near that - simply absurd.
Take today's number in NZ 3446 tests , 82 confirmed/positive , infection rate within the sample ~ 2.3%. If that rate held across the population we would have about 120K cases walking around - roughly 125 times more than the current confirmed tally of cases at 950. So what you are actually saying that the sample tested was representative of the population at large - which is clearly not the case as current selection criteria require symptoms / contact with confirmed case / travel etc. - which of course will make the infection rate within the sample MUCH greater.
I find it curious how all the talk is about infection rates and numbers and nothing of deaths. One so far and a long way to go to the tens of thousands predicted...
I find it curious that you effectively switch the topic ( from infection rates to death rates ) as soon as confronted with any actual numbers.
Deaths are of course a lagging indicator ( 2- 4 weeks for Covid19) ; so far most cases in NZ have been among international travelers and their contacts - a sample overweight in younger people which is also reducing death rates .
Normally deaths would make the headlines but with only 1 death in NZ so far, it's hard to support the apocalyptic narrative, so the media uses infection rates in their sensationalistic news to scare the gullible
If you think that's what's scaring people you might want to try thinking a bit harder.
Two weeks ago NZ had 52 confirmed/probable cases, now we have one death. thats a ~2% fatality rate with a two week lag.
For Australia it was 1072 cases, and now 28 deaths = 2.6%.
Assume 60% of the population gets it, and that 2% fatality rate holds true, 0.012 * 5m population = 60,000 deaths.
And in neither country have hospitals been overwhelmed yet. Try that simple analysis for USA, Italy or Spain (or pretty much any country with over 3000 cases) and watch the fatality rate increase.. because they can't test fast enough, and they can't treat the number of infected. so the infected count is low, and the number that die instead of recovering goes up massively. Denmark with 1326 cases two weeks ago, now 139 deaths. that is 10%. And they have a fairly comparable population to NZ.
Ludwig,
That paper you refer to was written on 17 March using data as at 16 March when US deaths were 68 according to the author. Now, 18 days later (American time) the American deaths are over 6000.
The author also uses the Daiamond Princess as an example, stating 7 deaths. But those deaths are now 11, with 15 people still either serious or critical. These people have now been ill for approximately two months and survivial rates for people who are sick with COVID that long are low. Also, there are questons as to whether all of the Diamond Princess patients have been correctly allocated to the Diamond Princess or to the countries where they were sent.
I imagine the author might be squirming a little now as to what he wrote back then.
KeithW
Italy and spain, the worst affected countries, have approximately 2 infections in 1000 people. Spain 120k out of 46 million. Italy 120k out of 60 million.
Sorry but NZ public have been fed highly sensationalised infection rates of 40 percent or OVERSTATED by 2000 percent. Lying statistics! Damn lies and statistics
Both those countries are under strict lockdowns to prevent the spread, and also the confirmed / reported cases are obviously a vast undercount of the number of people actually infected.
So yeah, of course the officially reported infection rate is much lower than the 'worst case scenario' - because no one is stupid enough to allow the worst case scenario to arise, nor are we even capable of confirming how many cases there actually are given the expense and limitations around testing.
Australia - only 5 deaths per one thousand infections
NZ - one death per one thousand infections
USA - 26 deaths per one thousand infections
World - 53 deaths per one thousand infections
Spain - 93 deaths per one thousand infections
Italy - 122 deaths per one thousand infections
Question: what is it about The Antipodes. The rates are based on actual numbers of sick people, nothing to do with not flu season
Too early to make any calls. It's so out of control in the US and Europe that testing has been grossly inadequate.
Other countries are testing much higher percentages than here. But if we prove that infection rate is understated that only goes to prove even more that the virus is not that lethal as what we have been told.
2 possible relevant variables: density of pop per square km plus median age of case of prison infected.
hence LA is much less bad than NYC
Houseworks
Death rates need to be compared with number of cases two weeks previously.
Also, NZ cases are predominantly either international travellers or people they live with. These people are in general not in the main risk categories for mortality.
Time will tell as it spreads out across demographic groups.
KeithW
Housework’s. Our lower rate could be because a) we are earlier in the curve than Italy or Spain, b) we put in place lockdown measures at an earlier stage than they did, c) other factors such as differing population density and more apartment living, family co-habitation patterns, demographics and a different exposure profile, such as more resilient younger people ( via returning travellers) getting infected here than Italy and Spain.
Australia - 218 cases/M people
NZ - 197 cases/M people
USA - 936 cases/M people
Spain - 2,699 cases/M people
Italy - 2,061/M people
To all commentators and keyboard "experts" - pull your heads in and be thankful you live here. I have a good friend in the thick of this at the MOH. They are working day and night and moving heaven and earth to make sure as few NZers die of this. They are very well qualified and bright people - they are doing the best they can and from what I see they are doing a good job - there could always be more of things etc and no one is perfect. The best thing people can do is follow the rules and we will get out of this in some form sooner rather than later.
Yes. We will soon be in less danger from Covid-19 than from drowning in the oncoming tsunami of hindsight. MoH does tend to be CYA, mother-knows-best, and don't-startle-the-peasants but those are problems more of style than substance.
Keith is correct to argue for much wider testing asap, I'd also argue for wide distribution/promotion of simple face masks before dropping from level 4 and I think that is do-able. I suspect MoH (aka Ministry of Not Panicking) is already considering both.
Hi JackL, in saying, "pull your heads in", does the silence you wish for include all those losing jobs, income, investments and those to pay for future taxes? Because that will be the majority the longer this draws out.
The beatings will continue until morale improves
Yes. It really is not the time to demand better from people who are both stressed and stretched. They are doing an amazing job in so many areas, contact tracing being just one that comes to mind.
"Accordingly, these serology tests are excellent as a filter of cases which are probably ordinary flu but for which there is uncertainty. They can also be used with close contacts to identify those that need to be quarantined more stringently. Even more important, they can be rolled out as a surveillance program at the community level."
I'm a practicing doctor, and these tests, even when fully validated, will be of very little use to me in these situations. The tests will probably be looking for IgM, which is usually the first antibody made, and perhaps also IgG, which is usually made considerably later. The IgM response can take upto two weeks though it might kick in after around five days in a few cases. This means that by the time an antibody test is positive, a first generation case has probably spread the infection to two more generations, and by the time contact tracing is done on the second generation of cases, they will have already exposed a 3rd (and potentially 4th) generation. Nor are these tests useful as a surveillance program at community level in real time, rather they are useful as an after the fact assessment of how widespread infection truly was. The only way to do close to real time surveillance of viral illnesses at community level is with PCR testing, ie the type of swab currently being done. PCR is how influenza and other viral illnesses are monitored in winter months for our national surveillance program, and there is talk of Covid-19 being added to that panel (which currently tests for around 15 viruses) this year. A scenario to consider, it's August 2020, there have been over 4,000 PCR confirmed cases around New Zealand, and I run an antibody test on a patient, in a city which has had several hundred confirmed cases. The patient attends on day four of illness, unwell with upper respiratory symptoms. Will a negative antibody test help me diagnose this illness? Not at all at this early stage, but a PCR swab would. Will a positive antibody test help me? It could only tell me whether the patient has been exposed to, and at least started to fight off, the Covid-19, but not whether their current illness is Covid-19 or something else. With several hundred known cases in my theoretical city, it's probably just as likely that the patient was exposed to Covid-19 two months ago as that their current illness is Covid-19. Again the PCR test would be far more clinically useful as it tests for active virus at the time. You rightly talk about antibody tests being used to estimate whole population immunity, and that is the only role I expect them to play. I hope we can eliminate this illness, but am not nearly as confident as you that we have a realistic chance to do so, far more likely we'll manage to suppress it, and have sporadic outbreaks. If we as a nation intend to suppress it until a vaccine is available, I hope we are ready for the length of the battle and the scale of other problems the economic damage gradually causes.
Thanks,Vivid.May I ask, when would you come out of national lockdown [if you were Prime Minister]?
As a doctor, you are saying: 1/ this virus will not be stamped out 2/ it will be a long battle 3/ there is going to be drawn out and voluminous carnage economically
Vivid,
The best antibody test kits combine IgM and IgG. I think you will get an IgM response quicker (earlier in the infection cycle) than what you are expecting here. And that changes many things. PCR surveillance programs come into play in terms of the value of information therein when the prevalence is higher. Serology testing comes particularly into play when we are still trying to stamp out rather than manage.
KeithW
Vivid, thanks for your comment, it's great to hear from a professional in the industry. I wish we had more more posts from professional people who know what they're talking about vinstead of uninformed opinions and immature arguments
Totally agree Yvil...this comment was posted yesterday by someone...."don't take others hostage to prolong your own life"
Would not like to be in a lock down with this individual.
Keith, I concur absolutely with your suggestion that the Queenstown conurbation be used as a whole-population test. Reasons:
- There are only three roads in and out: Crown Range, Kawarau Gorge, South to Lumsden. Easy to block them, test all ins and outs, and have a decent chance of a stable population.
- It's a very diverse population: everything from youngsters, through the 20-40 group who used to work in that recently deceased industry (tourism), to retirees dotted through the lifestyle blocks and the leafy lanes of Arrowtown. So it's probably sufficiently representative to be useful.
- It has easy, safe, secure air links for the necessary medical and specialist staff to travel to and fro on, and to transport samples etc as needed.
- It's probably a manageable size in terms of actually getting around a very high percentage of the inhabitants.
Your thoughts? A good science experiment in the making?
Waymad
Yes, based on experiential evidence from Vo in Italy, then if you can test a whole community you can stamp it out. Queenstown would be ideal because of the physical geography, the demographics, and the likelihood there is already community transmission going on within that community. You could do it with PCR but much more practical with quick-fire serology.
KeithW
Mike Hosking's various contradictory non-partisan driven views on Covid-19.
https://www.rnz.co.nz/national/programmes/mediawatch/audio/2018741210/m…
Thanks, I always go to Mike for a high quality news source.
You're lucky hot chocolate doesn't stain, or you'd owe me a new shirt...
As usual Keith your comments smack of long experience, expertise and common sense. Why haven't they chosen you to be on the co-party committee....I forget what they call it....instead of the likes of Simon Whinges whose background as a prosecuting lawyer debars him from anything to do with scientific proof and facts.
Keith, could you please tell us what you think of the "Swedish Experiment" whereby there is no lockdown.
Streetwise
I don't think the Swedish experiment is working. They have already had >350 deaths. That is a lot for a smallish country of 10 million and I expect to see those numbers increase considerably - at least fourfold, and maybe more, over the next two to three weeks. Sweden, Belgium and Netherlands all have per captia figures that look very worrying. Aso, I dont think Sweden is recording mild cases. Unless we are underestimating the herd immunity effect, which I think is unlikely, I can only see trouble for Sweden and the likelihood they too will belatedly end up in lockdown but from a very poor starting point.
KeithW
https://www.worldometers.info/coronavirus/country/sweden/
The last few days they've been getting about 500 new cases per day and 50 deaths per day. If that's the worst of it for them, then maybe the approach could be considered a success. But their curves look a bit worrying, so unfortunately there's a significant chance they're in for a tougher time over the next few weeks.
This comment posted by a facebook friend. He gave me a ride hitchhiking and we've become good friends. He has a science degree and works in a managerial position overseeing hospital testing over several regions. English isn't his first language, but he does pretty well.
I listened to today’s COVID19 midday update with great interest, especially the repetitive use of words like curve, peaking, flattening, rolling average, good level…It wasn’t difficult to identify the ‘spin’ related to laboratory testing, with tired unquantified lines like; increased testing stock, increased level of testing, enough componentry for the full testing process and increasing confidence in our ability… The reality is that not enough testing had been completed for diagnosis or to determine the flexion point for COVID-19. Therefore, it may not be wrong to theorise that the low number of testing is directly due to insufficient nasal/throat swabs and insufficient number of extraction kits available for RNA/PCR analysis. So, Minister, I don’t believe you!!
the key difference between the current antigen test and the antibody test proposed here is the antigen test only identifies whether someone is currently carrying the virus and is actively infectious. The antibody test identifies if someone has been exposed to Covid-19 and recovered.
JKB
Not necessarily recovered.
But the ratio of IgM to IgG may indicate the likelihod of the infection being current.
KeithW
If the lockdown was being executed 100% then we wouldn't even need testing as this virus would die out in a month. The problem is people and they just dont get it. Potentially if everyone had worn decent PPE then lockdown need not have happened at all. Reality is that lockdown simply cannot continue until the point a vaccine is available. What you have to hope for is coping a low viral load during a controlled release and just get over it while the hospitals run at near capacity. The testing that is now of more interest is those that have had it without even knowing it and have recovered. These people need a "Green Card" so they can get back to work now before the economy is so destroyed there is nothing to go back to.
Kieth a good article but i disagree with the following.
"To date, I have seen no mention from the Director of Health, nor any questions from the mainstream journalists, as to what New Zealand is doing in regard to serology testing.
I suspect the reality is that we are doing very little."
See the following Report Dated: 26-29thMarch 2020.This report was Commissioned By:The office of the Prime Minister’s Chief Science Advisor and can be found here https://cpb-ap-se2.wpmucdn.com/blogs.auckland.ac.nz/dist/f/688/files/20…
Report Recommendations:
•Recommendation#1: As much resource as possible should be targeted at monitoring and executing testing capabilities. This all-of-government response should include:(i) a COVID-19 PCR task force and; (ii) a COVID-19 ‘antibody/antigen’ task force. These groups should urgently coordinate purchasing, validation, funding requests, timelines, priorities, adoption and scope local (New Zealand-based) capabilities and expertise.
•Recommendation#2: New Zealand should continue to prioritise its PCR testing capabilities. Securing supply lines, scalability and speed of testing should be the country’s primary diagnostic focus at this point in time. Other countries are ahead of New Zealand on the infection curve and we are behind them in the queue for already scarce material for the test.
•Recommendation#3: New Zealand should actively engage with the rapidly developing ‘Point-of-care’ (POC) lateral flow diagnostic space for virus antigen and patient antibody (see inset image as an example). Purchasing decisions may need to be separated from adoption decisions to preserve optionality. There are risks in adopting the ‘wrong’ test that performs poorly–valuable resources may be expended if poor decisions are made.Conversely,there are risks of delaying decisions and missing out. The role and utility of new POC tests must be carefully explained to the public to avoid unrealistic expectations and perverse outcomes (e.g. patients who think they are immune, but are not,as the result of a false positive test for antibodies)
.•Recommendation#4: New Zealand should rapidly pursue testing capability to detect antibodies in a laboratory setting. Tests for antibodies in New Zealand’s diagnostic laboratories (a test called ‘ELISA’) should also be considered for large scale serological testing in the coming weeks. It is likely these tests will be deployed with only partial validation. These tests can be purchased from overseas suppliers but New Zealand laboratories are already working on generating viral proteins and antibodies needed for these tests. Coordination, funding and support for these New Zealand-based initiatives should be mobilised to prevent fragmentation and duplication. Report Key Messages:•Reliable and rapid testing for SARS-CoV-2 is a vital part of New Zealand’s pandemic response.•The primary method for virus detection is a testing method called the Polymerase Chain Reaction (PCR). As the World Health Organisation notes,this test is still the best way to track and trace virus. New Zealand must do everything possible to maintain (andoptimise) this testing capability. Securing supply chains of reagents must remain a top priority.•Losing our PCR testing capability would have catastrophic consequences. The volume of tests required now, and in the future, needs to be constantly monitored. •Testing can perform two vital roles in this pandemic:o(i) diagnosis of COVID-19 early in infection; this is undertaken using either PCR tests (current standard) or direct tests for virus particles (that are in rapid development but unproven)
o(ii) population antibody tests: identification of patientswho have been infected for some time or have recovered (and can possibly return to work) -antibody tests are new to market but are commercially available.•Advances in diagnostic testing are rapidly evolving -companies are developing tests and are pushing for adoption (and market share). Many of the tests are unproven. A watching brief on testing development should remain a priority so that New Zealand can respond and pivot if/when needed. •Recent articles in the media highlight a POC tests (akin to a pregnancy ‘stick’ test –called a lateral flow test –see image above) that can either (i) detect viral particles (called antigens) or (ii) detect antibodies that patients form in their bodies between 4-20 days after COVID-19 symptoms are first observed.•Tests to directly detect viral particles (called antigen tests) could be a replacement for our PCR testing. They are currently being validated prior to being deployed in the UK. However, such a test recently failed in Spain where, anecdotally, the test was only 30% accurate. While these tests are ‘in development’ they are not market ready (as of 29thMarch) and so have unknown specificity or precision. Adopting a poor test would have a very detrimental outcome during the track & trace pandemic phase.•Antibody testing (POC or laboratory based) will become increasingly useful in the New Zealand pandemic response, with antibody testing becoming a crucial part of testing hospitalised patients. There is a high chance that accurate antibody data generated in laboratories will enable us to better predict disease progression (and demand on hospitals). •It is vital that antibody tests (in contrast to antigen tests) should never be regarded as a replacement for PCR tests –they are complementary and serve a different purpose. The false positive/negative rates of these POC tests remain uncertain.•Antibody POC tests that identify past exposure are not very useful at this point in New Zealand’s current track & trace phase because of the time it takes for our bodies to mountan antibody response to COVID-19. This ‘time-lag’ makes these kinds of test a poor proxy for infection relative to current PCR tests. However, securing these tests for later phases of the pandemic should be considered a priority. •Testing for antibodies will almost certainly require the purchase and import of testing kits. There is an inherent risk that supply chains may become compromised and some companies may not be able to keep up with global demand. Events mean that procurement decisions will likely need to be rushed with multiple choices pursued to create a hedge strategy, but they must still be carefully considered and weighed against the risk of missing the window of availability. New Zealand should also mobilise its internal capabilities to develop and validate reagents used in COVID-19 testing reagents.
Authored By:Professor Michael Bunce Dr Marie Estcourt Input and Peer Review:Professor Rod Dunbar Mark Stuart
Acknowledgements:We acknowledge valuable input of; Susie Meade, George Slim, Ian Town and Juliet Gerrard Commissioned By:The office of the Prime Minister’s Chief Science Advisor (PMCSA)Contact regarding this report should be directed via the PMCSA’soffice: Phone+ 64 9 923 6318 Email: info@pmcsa.ac.nz
Thanks, Steve1.
Steve1
Very good to see this report. It seems to have received no publicity. Recommendation threee which starts "New Zealand should actively engage with the rapidly developing ‘Point-of-care’ (POC) lateral flow diagnostic space for virus antigen and patient antibody..." aligns exactly with what I have been advocating. The question now is whether the MoH is responding to this report and have they set up a taskforce. The report only came out a week ago, which in some contexts is very recent, but COVID-19 travels a long way each week! And the report does talk about the need to act very quickly, albeit with some hedging of bets.
KeithW
Why the ducks and drakes approach, Keith?
For example, I have seen a quote from a New Zealand firm, already working with Government on another project, that can supply these at under $7 per test, with 100,000 tests delivered within a week. One further week, and everything could be operational.
Surely that company would not mind you naming them - and if they want to sell something to the government that we are possibly all going to be tested with, we deserve to know who the heck they are. If you say they signed an NDA with the government - then what are they doing showing you a copy of their quote?
And more to the point, why are you, if you have knowledge of an NDA, making public this veiled 'fact'.
Are you just keen to imply you have insider information that you are unwilling to divulge to the rest of us?
Kate
It is always disappointing when people choose to get personal.
Actually, there are a number of companies who are pitching or would like to pitch to Government. But there is no taskforce for them to talk to.
My intention in regard to the specific paragraph which you take offence to was simply to indicate the scale, scope and issue of cost in broad terms.
I thought that would help people's understanding.
I intend to comment no further here in relation to your criticism given that you chose to make the issue personal.
KeithW
I am sorry for getting personal. I am like many in this lock down situation, overly emotive/emotional at this time. We all have friends and loved ones the world over, so it's not just 'the local' that contributes to my concers.
If I can explain my concern more rationally, it is this: I believe academics, in particular, need to be careful when straying outside their area of expertise in emergency/crisis situations. Especially when directing criticism at the government's efforts, there is a high bar of research needed when forming opinion pieces. Particularly when the issue discussed is already being addressed by government by those tasked to research the issues with those who have the requisite expertise, such as the PM's Chief Science Advisor and Dr Siouxie Wiles;
https://www.pmcsa.ac.nz/what-we-do/publications/
https://thespinoff.co.nz/science/31-03-2020/covid-19-what-difference-ca…
" I believe academics, in particular, need to be careful when straying outside their area of expertise .." - ahem.. pot - kettle - back . Women's studies anyone ?
Woman's studies - not me, I know little about that discipline overall, nor the principle methodological framework of critique;
https://owl.purdue.edu/owl/subject_specific_writing/writing_in_literatu…
Ok , let us grant this.
So what is the relevance of your "expertise" to epidemiology ?
None whatsoever. I'm not the author of the article.
A see ; it only applies to writing articles , not commenting on them.
And here is Kate ( a tutor at Massey University's College of Humanities) penning an article on among other things bottom trawling synthetic nitrogen, agricultural emissions etc. etc.
Short or selective memory ?
Next time you decide to try and shoot the messenger take better care not to shoot yourself in the foot ...
https://www.interest.co.nz/opinion/102433/katharine-moody-government-op…
paashaas, I see Top 5 guest contributions quite different. The format is: link to an article of interest, quote from that article, and then express an opinion, if I have one. I've never been the author of any of those articles linked to, nor do I claim to have particular expertise in those areas - that's why all the links!
In fact, I find interest.co.nz reader/commentators often have far greater knowledge than I do in many of the subjects discussed. For me, this site is a place of learning.
I get it - of course it is QUITE different when Kate writes it. Her hart is pure , her politics "progressive" . It is like .. you know . . DIFFERENT.
That I see it as different, doesn't mean you see it as different. I get that. It's what blogs are all about.
Kate,
I can confirm to you that I have experience working with antigens, antigens, PCR and ELISA, and the interpretation of results, and also with infectious disease eradication and computer modelling. I also confirm to you that I read the scientific journal articles on matters that I write about. Although the media likes to talk of experts, the reality is that in these matters we are all learners. As learners, we all have to learn to take criticism on the chin as long as that criticism relates to technical errors or errors of exposition. One of the challenges we have here in NZ (and elsewhere) is that the general population has very little knowlege of science, yet these are matters that affect the lives of all of us.
KeithW
It's not technical errors by any means that I believe you have made. It's lack of understanding of the Government's exploration on the issue already done at the time you wrote the article (i.e., CSA publication 30 March; commented on by Dr Wiles on 31 March; your article published 4 April) and your failure to provide links to support your evidence (e.g., the company in NZ that makes these products).
As you have acknowledged, you didn't know about the CSA publication when writing your piece, what I'd do is a strike-through of your article above, to correct inaccuracies as at the time of writing, for example this one;
To date, I have seen no mention from the Director of Health, nor any questions from the mainstream journalists, as to what New Zealand is doing in regard to serology testing. I suspect the reality is that we are doing very little.
That situation may be linked to the reality that most Ministry of Health staff will be pre-occupied with operational issues. Ministry of Health is unlikely to have many staff with serology expertise. These types of people tend to not be found in the bureaucracy.
Accordingly, it is time for our Prime Minster to ask the Ministry of Heath to set up a group to report back within 72 hours as to the pathway forward. Alternatively, the Prime Minister’s Chief Scientific Officer could be tasked to manage this.
Kate
It is always disappointing when people choose to get personal.
Actually, there are a number of companies who are pitching or would like to pitch to Government. But there is no taskforce for them to talk to.
My intention in regard to the specific paragraph which you take offence to was simply to indicate the scale, scope and issue of cost in broad terms.
I thought that would help people's understanding.
I intend to comment no further here in relation to your criticism given that you chose to make the issue personal.
KeithW
5 day delay on local lab testing results as numbers of tests rise.
evidence?
Local laboratory email. Cannot keep up with demand.
What local lab, and what tests are they talking about be? Can we quit it with the vague rumors, be specific.
Yes, I agree Pragmatist. In view of delivery by the PM of her decision to continue or not the current lockdown, 5 days is a long time to delay for current epidemiological data....almost a week old. A week in a 4 week lockdown. But what does it matter whether it is BS or not? I could be making it up, but I am not. It is likely that other regions are similar. Let's face it, we are not prepared with sufficient quantities of PPE, respirators, Medical staff, etc, let alone full on lab testing capability. Waikato. Covid nasopharyngeal viral swab. But there is enough worry, so I did not want to be specific. Only to point out that faith in the stated statistics can be misplaced.
" But there is enough worry, so I did not want to be specific."
So you threw out some completely unfounded fearmongering crap. Either back it up or shut up.
Since apparently we are only testing at a fraction over half our national capacity according to todays press conference, this seems completely improbable. Its a two hour drive from Hamilton (which i assume is the centre doing most of the testing) to Auckland. Why are they not driving/flying the excess samples to Auckland, or another centre with more capacity?
Dr Siouxsie Wiles, Associate Professor and head of the Bioluminescent Superbugs Lab at the University of Auckland comments on the same subject;
https://thespinoff.co.nz/science/31-03-2020/covid-19-what-difference-ca…
Hot off the press from Lance O'Sullivan. Outrageous situation in Kaitaia. Sick people he is finding on the streets and he can't test. https://www.facebook.com/lance.osullivan.16/videos/10157127141803803/?t…
Following O'Sullivan's video, the Northland DHB posted online confirming the testing clinic running out of the whare at the front of the hospital ran Monday to Friday, 9am to 4pm. However, in the post, which the DHB said was a "truthful message", the hospital's operational manager Neta Smith said there were other services operating.
"After-hours in Kaitaia we have GP services and hospital services running 24 hours 7 days per week. If someone is unwell and they need to be seen they will be seen and tested," Smith said in a video.
"Anyone with acute respiratory infection and at least one of the following symptoms: cough, sore throat, shortness of breath, head cold, loss of sense of smell, with or without fever will be tested for COVID-19."
She also pushed back on any suggestion that there was only four swabs at the hospital.
"We have adequate supplies and equipment to treat you and currently have 120 swabs available in Kaitaia Hospital," she said.
"We do not need two testing centres in Kaitaia but we may need to transition to another site in the community if Kaitaia hospital gets busy with COVID-19 cases.
"The best thing you can do is stay home and remember if you need GP or hospital services please do not hesitate to call us so we can see how best to help you."
There are no confirmed or probable cases of COVID-19 at Kaitaia hospital. There are seven community testing stations throughout Northland.
Nice bit of rhetoric. How can they test without test kits? Also ignores the fact of a probable active case that just spread it around a supermarket.
The swab (and related vial) is the test kit at that end of the chain, the test kit as such is in the Laboratory, where ever Northland DHB sends it samples.(probably Whangerei, possibly they get driven to Auckland?)
He talks about Swabs. He is a doctor, I think his complaint is legitimate & accurate.
Yes, he talks about swabs, and the MoH has come out and said there are 120 at Kaitaia Hosp. YOU brought up test kits. Test kits are not swabs. It's not at all clear his complaint or yours are valid.
A haka would sort it out
DP
Nope, I didn't say test kits, I said he couldn't test. Really I just introduced the video, he talks in the present tense.
"Nice bit of rhetoric. How can they test without test kits? Also ignores the fact of a probable active case that just spread it around a supermarket."
Yeah.. you did.
The government should have done two things to help slow the virus
ALL overseas KIWIS and tourists have to stay where they are.
ALL returning overseas kiwis and tourists be quarantined for two weeks by force if need be.
We would probably be at lock down 3 not 4, the damage to the economy would have been far less.
Ardern needs to show she is a true leader
A proposition for coming out of the level 4 lockdown:
Keep the strict lockdown for people over 65 who 1) are at greatest risk of death 2) are no longer in the workforce
Have a soft lockdown for the working population, i.e. keeping businesses open under certain rules (social distancing, wearing masks, latex gloves, limiting number of people in groups), thus still limiting the spread of CV, protecting the elders but saving businesses and jobs.
Your thoughts?
it might have legs - but a bit too early to say.
Critical developments to watch over the next few weeks :
- how well or badly current NZ"semi-hard" lock down is working
- how well "soft" lock downs similar to what you suggest are working elsewhere
That's pretty much what Alert Level 2 is;
https://thespinoff.co.nz/politics/21-03-2020/covid-19-nz-live-updates-m…
Don't worry Keith, it's all over, a cure has been found:
https://www.tvnz.co.nz/one-news/world/australian-study-finds-common-ant…
What can't the Aussies do in medicine; I have been watching the Australian Sky News over the past months and those remarkable Aussies have reported their cures for all the major diseases: heart, asthma, cancers, you name it!
Huh? sounds a bit too easy to good to be true, Keith you view?
Streetwise and Yvil,
This is not as far fetched as it might sound.
Ivermectin is already aproved for use in humans for other purposes ( internal parasites) and is generally regarded as safe but with some provisos for particular situations.
The people doing this work are competent people of integrity.
And the lab results are very strong.
But it needs now to be undertaken in people.
Here is a link to the full paper.
https://www.sciencedirect.com/science/article/pii/S0166354220302011?via…
KeithW
Peak Prosperity
Q: anyone know if/why it was one guy, one bat, one bowl of soup?
Henry-Tull
Yes, this is a particularly good video, albeit long, for those who are interested in virology, which is a key part of the overall story, but which is different to the epidemiology. The first 40 minutes is probaly the most informative part.
KeithW
Is this patient Zero?
The YouTube video then mentioned that Mr. Xiao of the South China University of Technology had identified Ms. Huang as Patient Zero who became infected during a laboratory accident and later died. The report said the virus was transmitted to the public by staffers who attended her funeral.
https://m.washingtontimes.com/news/2020/apr/4/us-scientists-say-china-h…
This would explain why it's not multiple animals, transmissioning to multiple people.
The P4 lab.
Different to the CDC P2 lab.
The virus hunters need to know if its
Bat to person
Or
Bat to anteater to person.
And natural jump, yes/no.
It's a big deal if it's from the lab, and Not the Wet markets.
Another Interesting summary of worldwide progress (or regress) (excluding China, whose data simply cannot be trusted). from Christopher Monckton of Brenchley.
This particular situation shows just how useless most governments are. The public health crisis started years ago and continues today. Big business has been pedaling the most toxic and sickening products to the public, even though their effects are known. If you have been to the USA you will have seen some of the fattest and sickest people in your life. Restaurants have sharp containers in the bathrooms for all the insulin needles. The USA produces more than 4,000 calories per person per day. Lots of profit!
In Japan they have the Metabo Law which requires men and women between the ages of 40 and 74 to have their waist circumference measured annually. This is not fat shaming, these people have a health issue. The latest Covid stats from NYC clearly show the chickens have come home to roost.
Have a look at the fizzy and chip shelves at our supermarkets - all empty. Covid could rip through certain areas of NZ like the US. Some people are too dumb to make healthy choices, but hey we don't won't to upset the Cola investors.

We welcome your comments below. If you are not already registered, please register to comment
Remember we welcome robust, respectful and insightful debate. We don't welcome abusive or defamatory comments and will de-register those repeatedly making such comments. Our current comment policy is here.